Home » Medical Camera Benefits
Medical Camera Benefits
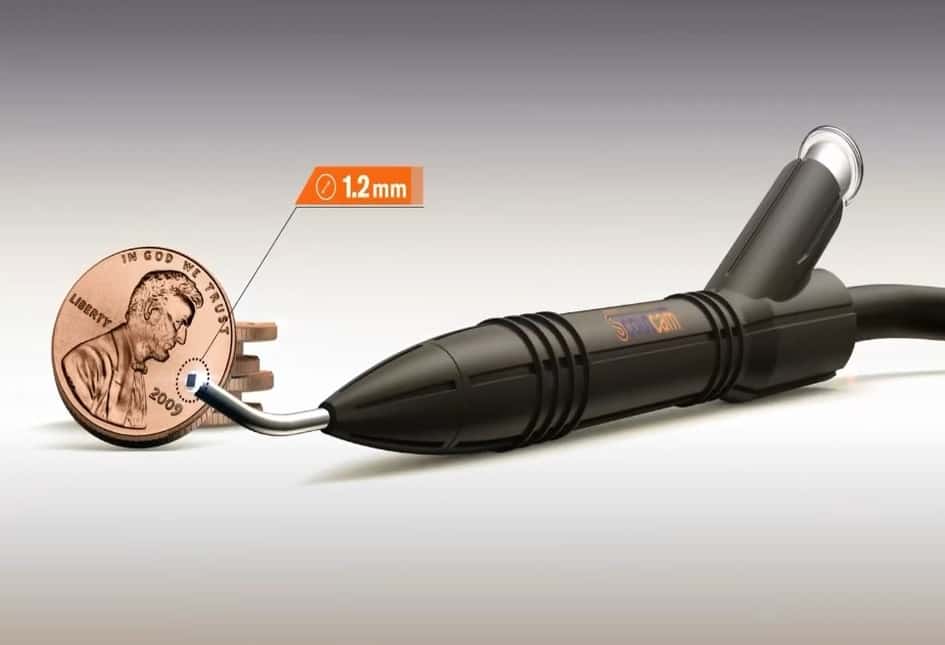
Thanks to continual advances and miniaturization, today’s sophisticated medical cameras can see where our eyes cannot: for diagnosis, delivering therapy, performing surgery, as well as researching tomorrow’s treatments. We and our loved ones are experiencing the impact of these highly complex imaging devices, some of which are the smallest and most durable cameras in the world.
Driving Forces Behind Medical Camera Market Growth
As reported in Nasdaq.com, there is increased investment in medical supply companies as a result of the COVID-19 pandemic. Disruption and innovation megatrends are fueling advances in imaging and medical camera technologies and platforms. In particular, the future of the medical camera market looks promising with opportunities in hospitals, diagnostic centers, specialty clinics and ambulatory surgery centers. Data indicates that amid the pandemic, the global market growth for medical cameras is now estimated at $3B and projected to increase to $5B by 2027. Notably, the surgical camera system segment is projected to increase at 7.7% compound annual growth rate (CAGR) for the next 7-year period. The major growth drivers for this market are the increasing number of surgical procedures that utilize medical cameras, rising R&D expenditure and technological advancements in medical cameras.
There has been “significant growth” in the endoscopy segment due to the several factors:
- Rising demand for minimally invasive surgeries
- Increasing prevalence of diseases such as arthritis, cancer and cardiovascular diseases
- Wide spectrum of use for the GI tract, the respiratory tract and other procedures such as laparoscopy, arthroscopy, cystoscopy, obstetrics, bronchoscopy, laryngoscopy, mediastinoscopy (usually for the purpose of obtaining biopsy, diagnosing/staging lung cancer, diagnosing lymphoma), evaluation of dental restorations, and others clinical applications
Technology-wise, digital imaging (2D/3D) has the largest market share, with the advantages of instant examination of the images with no film purchase and development costs. Today’s biomedical research also relies on digital images and videos from medical cameras to visually document clinical studies as well as microscopy findings.
How Do Medical Cameras Work?
Of utmost importance: All medical cameras introduced into the body must be strictly clinically proven for biocompatibility and safety in accordance with regulatory requirements. Illumination and irrigation features are often integrated with camera hardware to assure uninterrupted delivery of clinical images.
Following is an overview of how some medical cameras and their imaging components work:
- Lensless, ultra-miniature CMOS computational imagers and image sensors employ special optical base gratings integrated with Complementary metal–oxide–semiconductor (CMOS) photodetectors. Because such imagers have no lens, they are ultra-miniatureand have large effective depth of field (1mm to infinity). This tiny size is highly suitable for endoscopy and medical sensing, as well as medical camera inspection applications. Additionally these high-performance imagers are inexpensive making them ideal for integration in cost-effective, disposable / single-use medical devices.
- Miniature cameras
o Fiber-based (though thin, optical fibers are breakable and therefore can’t access many spots. Can be costly – the smaller the diameter the higher the price
o Camera-at-tip solution integrated in flexible or rigid endoscopes
o Embedded within medical capsules (“pill-cams”) a disposable medical camera inspection / diagnostic tool with 1-2 video cameras with restricted battery life; transmitted images are processed and viewed later, not in real-time, via specialized software - 3D medical imaging cameras uses laser triangulation, structured light or stereoscopy for capturing and rendering 3D information; applications can include 3D-toothscanning for dental restorations, simulations of cosmetic surgery
- Infrared imaging uses various wavelengths to visualize water content, temperature or chemical components of tissue which cannot be detected with conventional medical inspection cameras.
What happens to medical camera images and videos once they are created? Since today’s medical cameras product large amounts of digital data, there are global standards such as the Digital Imaging and Communication in Medicine (DICOM) Standard for storing, exchanging and transmission. DICOM uses image-compression and streaming standards and protocols such as the JPEG 2000 Interactive Protocol (JIP). Camera output is stored digitally on-premise or in the cloud via Picture Archiving and Communication Systems (PACS).
Benefits of Medical Machine Vision Cameras
Machine vision is the technology using medical inspection cameras and methods to provide high-performance, high-precision augmented visualization and image-based analysis.
Components include hardware and software: a single medical camera or cameras, lens, lighting to ensure the image is clear, frame grabber along with computer and software to analyze and process images, pattern matching and other algorithms may be used, according to the nature of images analyzed. Output components can be a screen for presenting data as well as mechanical components such as a robotic arm, for example.
The AIA Global Association for Vision Information notes that medical machine vision cameras “can also automate tasks like inspecting slides of a patient’s cells for tumorous cells or for finding areas of concern, drastically reducing the amount of time the process takes and potentially increasing the accuracy of the results. Medical cameras also facilitate simpler, easier documentation and monitoring over time.”
Conclusion
Growing investment in medical camera technology and increasing market needs will continue to fuel innovation. Cost-effective micro-camera technology is already meeting emerging demands, such as for disposable/single-use endoscopes and minimally invasive devices with superior visualization capabilities. Advances in medical machine vision will continue to enhance clinical image analysis. Such developments https://www.odysight.ai/articles/industrial/micro-cameras-bring-new-video-applications-into-focus/will help make diagnosis faster, more accurate, and surgeries more precise and less invasive.